Medigap Plan G with guaranteed issue rights is one of the most valuable protections available to Medicare beneficiaries. This combination gives you access to comprehensive coverage without worrying about medical underwriting or pre-existing condition exclusions.
At Dave Silver Insurance, we’ve helped countless people navigate these enrollment windows and secure the coverage they need. Understanding when you qualify and how to act quickly can mean the difference between seamless coverage and costly gaps in your healthcare protection.
What Plan G Actually Covers and Why Guaranteed Issue Rights Matter
Plan G Coverage Details
Plan G stands out as the most comprehensive Medigap option available to people turning 65 after January 1, 2020. This plan covers your Part B coinsurance, copayments, and blood transfusions. It also pays 100% of your Part A hospital costs and skilled nursing facility care after you meet your deductible. The only significant cost you still pay out-of-pocket is the Part B annual deductible, which sits at $283 in 2026. For most beneficiaries, Plan G eliminates the financial uncertainty that comes with Original Medicare, where you’d otherwise face unpredictable bills ranging from thousands to tens of thousands of dollars depending on your health needs that year.
How Guaranteed Issue Rights Protect You
Guaranteed issue rights are your legal protection that allows you to buy Plan G without medical underwriting, regardless of your health history. This means insurers cannot deny your application, charge you more based on pre-existing conditions, or impose waiting periods for coverage. Medicare.gov confirms that when you have guaranteed issue rights, the insurer must sell you any Medigap plan they offer at their standard rates.
The Cost of Missing Your Protection Window
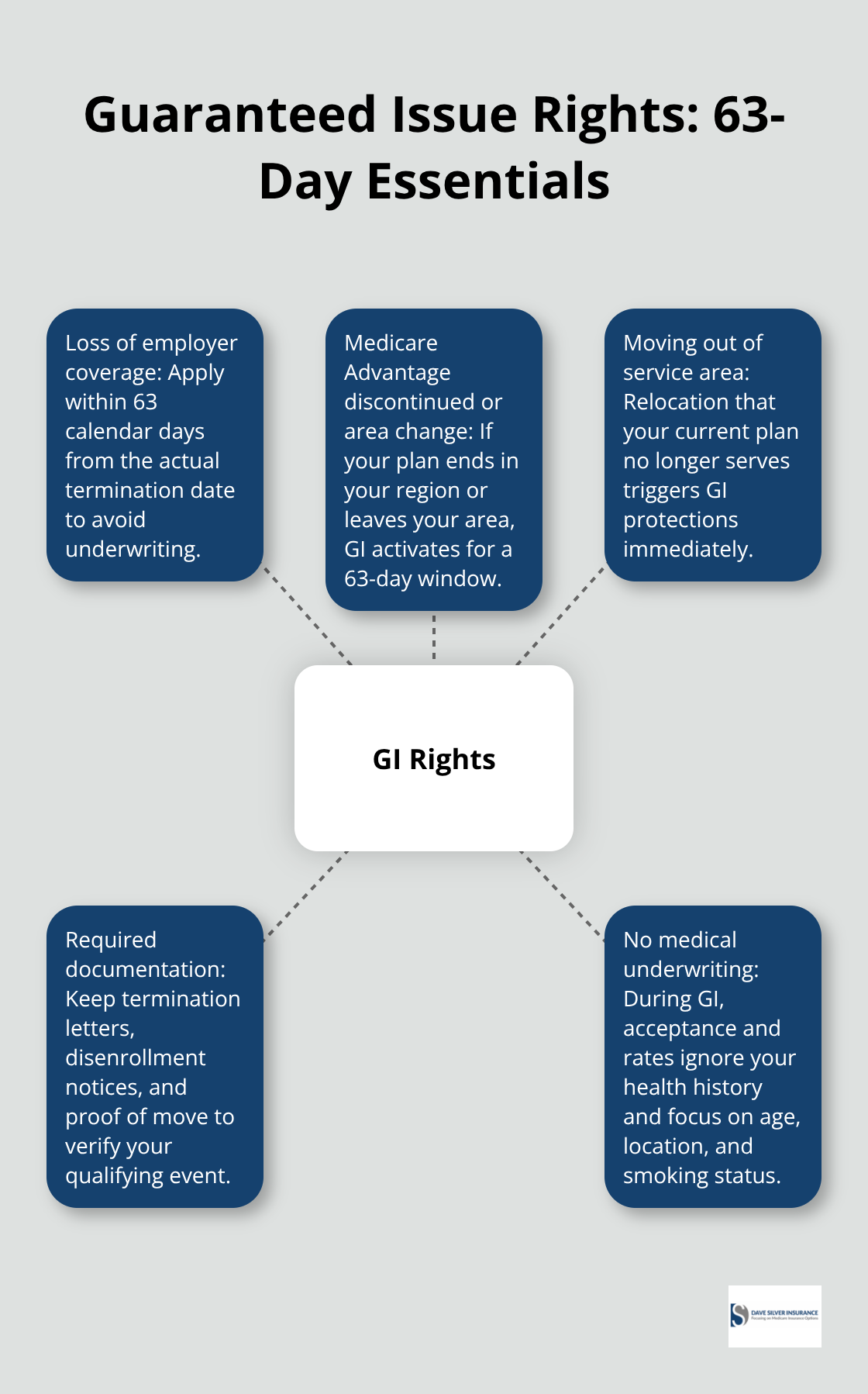
Outside of guaranteed issue protections, insurance companies can and will reject applications, charge substantially higher premiums for health issues, and apply six-month waiting periods for pre-existing conditions. Someone with diabetes, heart disease, or cancer who misses their enrollment window might face premiums 50% to 100% higher than standard rates, or outright denial of coverage. Guaranteed issue rights eliminate this risk entirely during qualifying events like losing employer coverage, having your Medicare Advantage plan discontinued, or moving out of your plan’s service area.
The number 100% seems to be not appropriate for this chart. Please use a different chart type.
Acting Within Your 63-Day Window
The window to use these rights is tight-you typically have 63 days from when your qualifying event occurs. Acting fast matters far more than taking time to shop around extensively. This narrow timeframe means you need to understand which events trigger your protection and what documentation you’ll need to submit your application quickly.
Qualifying Events That Trigger Guaranteed Issue Rights
Losing Your Employer Group Health Plan
Losing employer coverage remains the most common trigger for guaranteed issue rights, and the stakes here are significant. When your employer group health plan ends, you have exactly 63 calendar days from the termination date to apply for a Medigap plan without facing medical underwriting. Medicare.gov specifies that you need documentation proving when your coverage ended-keep your termination letter, final paystub showing benefits ended, or written confirmation from your employer’s HR department. The 63-day clock starts from the date your coverage actually terminates, not when you receive notification, so don’t assume you have extra time if your employer’s notice arrives late.
If your group plan was secondary to Medicare rather than primary, you still qualify for guaranteed issue rights, though the documentation requirements remain identical. One critical detail many people overlook: if you voluntarily left your job and lost coverage as a result, you may still be eligible depending on your state’s rules. States like Alaska, Arkansas, California, Colorado, Florida, Idaho, Illinois, Indiana, Iowa, Kansas, Louisiana, Maine, Missouri, Montana, Nevada, New Jersey, New Mexico, Ohio, Oklahoma, Pennsylvania, South Dakota, Texas, Virginia, West Virginia, and Wisconsin recognize voluntary termination as a qualifying event. Contact your State Insurance Department to confirm whether your specific situation qualifies in your state.
Medicare Advantage Plan Discontinuation or Service Area Changes
Your Medicare Advantage plan disappearing from your area or being discontinued by the insurer gives you another clear path to guaranteed issue rights. If your MA plan ends coverage in your region or your insurer discontinues the plan entirely, you have 63 days to enroll in a Medigap plan. Moving out of your MA plan’s service area also triggers these protections-if you relocate and your current plan no longer serves your new address, guaranteed issue rights activate immediately.
The documentation you need differs slightly here: obtain your disenrollment notice from your MA plan showing the effective date coverage ends, and keep any notices about plan discontinuation or service area changes. Moving to a new state or even a new county can trigger this event, so don’t overlook relocation as a qualifying trigger. These situations matter because they remove the insurer’s ability to underwrite your health, meaning your acceptance and rates depend solely on your age, location, and smoking status-not your medical history.
What Happens Next in Your Enrollment Process
Understanding which qualifying event applies to you sets the stage for your next critical steps. You’ll need to gather your documentation, understand your 63-day timeline, and prepare your application materials to move forward with enrolling in a Medigap plan.
How to Apply for Medigap Plan G When You Qualify
Contact Insurers and Submit Your Application
The application process itself is straightforward, but timing and documentation determine whether you succeed or face rejection. You contact insurance companies directly to request Plan G applications, and most insurers now offer online, phone, or mail submission options. When you call or apply online, inform the company that you’re applying under guaranteed issue rights and specify which qualifying event triggered your eligibility. This matters because the insurer needs to process your application under the correct rules. During guaranteed issue periods, insurers cannot use medical underwriting to accept or deny your application, meaning your health history stays completely irrelevant to their decision.
Most companies ask basic questions about your age, location, smoking status, and the date your qualifying event occurred. The application itself typically takes 15 to 20 minutes to complete, whether you do it online or over the phone. Many people unnecessarily delay this step by trying to compare multiple insurers when their 63-day window is closing. The better approach is to apply with one reputable insurer immediately after your qualifying event occurs, then worry about shopping around later if needed.

Understand Your Coverage Start Date and Backdating Options
Your coverage typically starts the first day of the month after your application receives approval, unless you request a different effective date. Some insurers allow backdating to the first day of the month when your qualifying event occurred, which can save you hundreds in out-of-pocket costs if your event happened early in the month. This backdating option exists precisely because of guaranteed issue protections-insurers cannot deny this benefit when you qualify under these rules.
Prepare Your Documentation Before You Apply
Documentation requirements depend entirely on which qualifying event applies to you, and having everything prepared before you call dramatically speeds up approval. For employer group plan termination, you need your termination letter showing the coverage end date, or a written statement from your employer’s HR department confirming when benefits ended. If your employer’s notice arrived late or you’re unsure of the exact date, contact HR directly and ask them to email or mail you official confirmation.
For Medicare Advantage plan discontinuation or service area changes, obtain your disenrollment notice from your MA plan showing the effective date. If you’re moving and your plan no longer serves your new address, keep documentation of your move such as a utility bill or lease agreement dated before you apply. The critical rule is that you must apply within 63 calendar days from when your qualifying event actually occurred, not from when you received notification.
Submit Documentation and Keep Copies Safe
Insurers will request copies of this documentation during the application process, so have scans or photos ready if applying online. Keep the originals in a safe place because some insurers may request certified copies later. One practical tip: call your state’s State Insurance Department before applying if you’re unsure whether your specific situation qualifies as a guaranteed issue event. They can confirm your eligibility and identify which insurers sell Plan G in your area, saving you time contacting companies that don’t offer this plan where you live.
Final Thoughts
Plan G stands as the most comprehensive Medigap option for people turning 65 after January 1, 2020, and guaranteed issue rights eliminate the biggest barrier to accessing it: medical underwriting. When you qualify under a guaranteed issue event, insurers cannot deny your application, charge more for pre-existing conditions, or impose waiting periods. This protection saves you thousands of dollars over your lifetime compared to applying outside these protected windows.
Your 63-day window closes whether you act or not, making speed your greatest advantage. Contact an insurer within the first week of your qualifying event, submit your application with proper documentation, and secure your coverage. You can always switch plans later if you find better rates, but you cannot recover Medigap Plan G guaranteed issue protections once that deadline passes.
We at Dave Silver Insurance help Medicare beneficiaries navigate these critical enrollment periods and understand the urgency of guaranteed issue deadlines. Contact us to discuss your specific qualifying event and get your application submitted before your protection window closes.
Disclaimer: The information provided in this blog is for general informational purposes only and does not constitute legal, financial, or insurance advice. Coverage options, terms, and availability may vary. Please consult with a licensed professional for advice specific to your situation

