Medicare stair lift coverage isn’t automatic, and many people don’t realize they qualify. The good news is that Medicare Part B does cover stair lifts when you meet specific medical requirements and follow the right approval process.
At Dave Silver Insurance, we’ve helped countless people navigate this system and get the equipment they need. This guide walks you through exactly what Medicare requires, how to submit your claim, and what to expect along the way.
What Medicare Actually Requires for Stair Lift Coverage
The Hard Truth About Medicare Part B
Medicare Part B does not cover stair lifts. This isn’t a gray area or a technicality you can argue around. Medicare classifies stair lifts as home modifications, not durable medical equipment, which is why the coverage door closes before you even get to the approval process. The distinction matters enormously. Medicare covers wheelchairs, walkers, scooters, and patient lifts when prescribed by a doctor because these are portable devices you use away from home. A stair lift attaches permanently to your staircase, making it a structural alteration to your house rather than medical equipment.
This classification has held firm since Medicare’s inception, and no exception exists for medical necessity. If someone tells you Medicare Part B will cover your stair lift, they’re mistaken.
Medicare Advantage Plans: Your Real Option
What might offer coverage is a Medicare Advantage plans, which operates under different rules than Original Medicare. Some Medicare Advantage plans have begun covering home modifications since federal rules changed in 2019, but coverage varies dramatically by plan and region. You need to contact your specific Medicare Advantage insurer directly and ask whether stair lifts qualify as a covered benefit under your plan.
Expect them to require a doctor’s prescription stating medical necessity, documentation from your physician explaining why climbing stairs poses a safety risk, and possibly an occupational therapist’s evaluation. Even then, approval isn’t guaranteed. The insurer will evaluate whether the stair lift prevents nursing home placement or hospitalization, which is the standard many use.
Building Your Medical Case
Your doctor’s prescription is non-negotiable if any chance of coverage exists through a Medicare Advantage plan. A casual conversation with your physician won’t suffice. You need them to document specific mobility limitations in your medical record that make stair climbing dangerous.
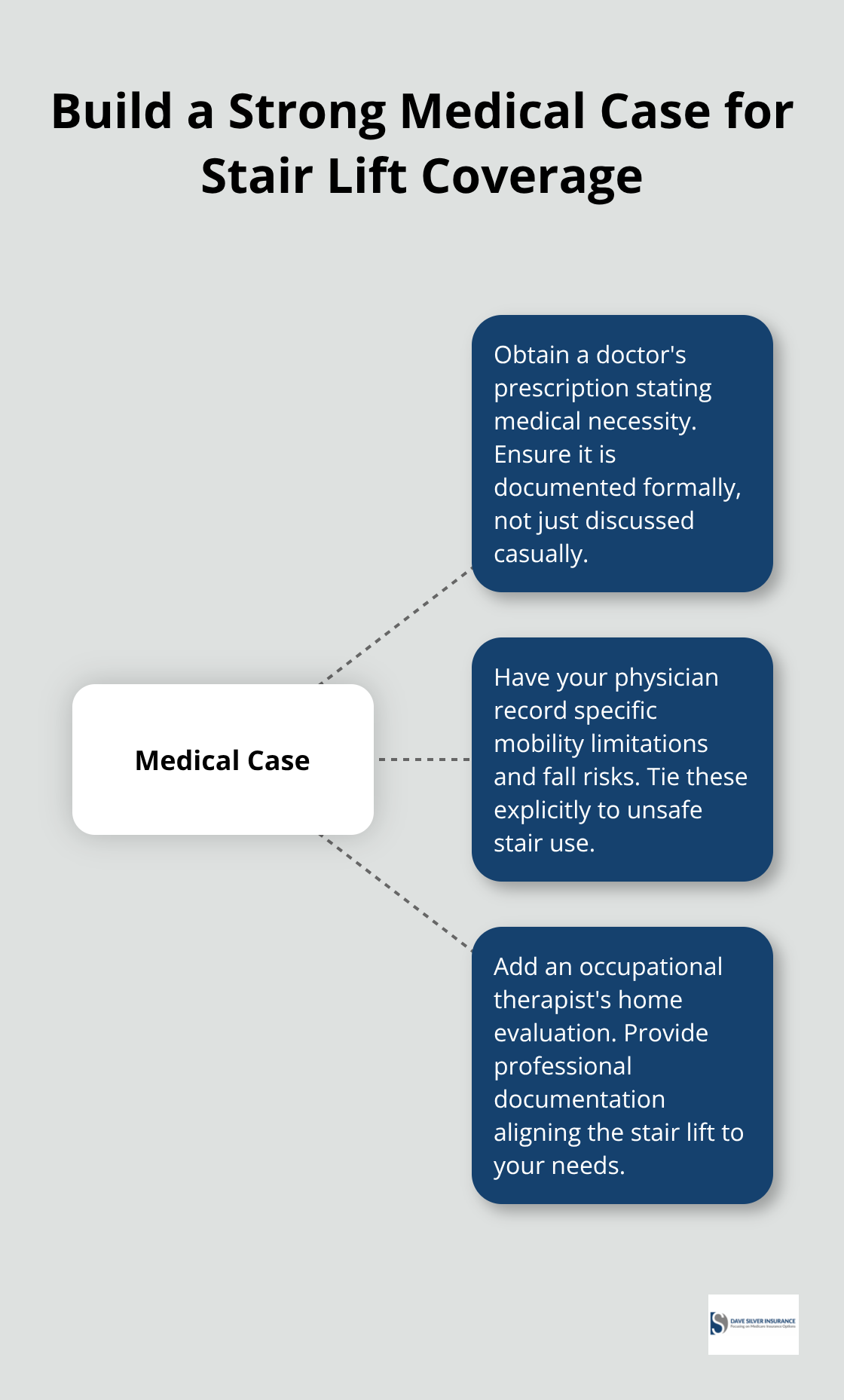
This means describing symptoms like severe arthritis limiting your ability to lift your leg, balance problems that create fall risk, or cardiac conditions that make exertion unsafe.
Your doctor should connect these limitations directly to why a stair lift is medically necessary, not just convenient. An occupational therapist’s evaluation strengthens your case significantly. They can assess your home, evaluate your transfer abilities, and provide professional documentation that a stair lift is the appropriate solution. This expert input carries weight with Medicare Advantage insurers because it demonstrates a thorough clinical assessment, not just patient preference.
Documentation That Insurers Actually Want
Gather all medical records showing your diagnosis, treatment history, and functional limitations. Insurance companies want evidence that your condition directly impacts your ability to use stairs safely. The more specific your documentation, the stronger your position when you submit your claim. Your physician’s notes should reference your specific diagnosis and explain how it prevents safe stair use. Medical records that show ongoing treatment and symptom progression demonstrate that your condition is real and documented, not a recent complaint.
Once you have your medical foundation in place, the next step involves understanding exactly how to submit your claim and what happens after you do.
Getting Your Medicare Advantage Claim Submitted and Approved
Confirm Coverage Before You Commit
Call your Medicare Advantage insurer’s member services line and ask specifically whether stair lifts qualify as a covered benefit under your plan. Coverage eligibility varies dramatically between plans and regions, so this conversation determines whether you proceed. Ask three concrete questions: Does your plan cover stair lifts, what documentation they require, and whether pre-authorization is mandatory before purchase. Many insurers require pre-authorization, meaning you cannot buy the equipment first and seek reimbursement later. Getting this wrong costs thousands of dollars out of your pocket.

Partner with Your Stair Lift Supplier
Once you confirm coverage is possible, work directly with your stair lift supplier rather than handling the paperwork alone. Reputable suppliers understand the Medicare Advantage approval process and know which documentation insurers actually demand. They submit your claim alongside the proper medical records, your doctor’s prescription, and the occupational therapist’s evaluation you gathered earlier. This partnership matters because suppliers submit claims correctly the first time, reducing delays and confusion.
Track Your Claim Through the Review Process
The insurer’s review typically takes four to six weeks, though some plans move faster. During this period, you should receive updates from both your supplier and the insurance company. If you do not hear anything within three weeks, contact your insurer directly and ask for a claim status update using your claim number. Silence usually means your paperwork is missing something or sitting in a queue. Follow up persistently because insurers respond to pressure and attention.
Handle a Denial and File an Appeal
If your claim gets denied, you have the right to appeal within 60 days. Request the denial letter in writing, which explains exactly why coverage was refused. Most denials cite insufficient medical documentation or the insurer’s determination that the stair lift is not medically necessary to prevent nursing home placement. Address these specific reasons in your appeal by submitting additional medical evidence from your doctor or a stronger occupational therapist’s report. For step-by-step procedures on how to appeal, visit Medicare.gov/claims-appeals. This second submission often succeeds where the first one failed because you now address the insurer’s stated objections directly.
Get Expert Help to Navigate Your Options
The Medicare Advantage approval process frustrates many people, and the stakes are high when thousands of dollars hang in the balance. An expert can review your coverage options before you invest time and money in the application process. Understanding whether your specific plan covers stair lifts, what documentation strengthens your case, and how to appeal a denial separates successful applicants from those who give up. With your claim either approved or moving through appeal, the next step involves understanding what costs you’ll actually pay out of your pocket and what other funding sources might fill the gaps.
What You’ll Actually Pay for a Stair Lift
Original Medicare Part B does not cover stair lifts, which means you will not receive the standard 80 percent reimbursement that applies to other durable medical equipment. This leaves you responsible for the full cost unless your Medicare Advantage plan includes coverage or you qualify for alternative funding sources. Straight stair lifts typically cost between $2,500 and $6,000 installed, while curved models for staircases with landings can exceed $30,000. Installation alone adds roughly $2,000 or more to the final bill, and professional installation is essential for safety and warranty protection.

Understanding Your Medicare Advantage Coverage
If your Medicare Advantage plan does approve coverage, read your plan documents carefully because approval rarely means 100 percent coverage. Most plans cover a percentage of the approved cost, leaving you with a copay or coinsurance responsibility. Contact your insurer for the exact out-of-pocket amount before you proceed with purchase. This step prevents surprises when the bill arrives.
Cost-Reduction Strategies That Work
Buying used stair lifts costs significantly less than new models, typically $2,000 to $3,000, but only if you purchase from a reputable dealer who has thoroughly inspected and reconditioned the unit to original specifications. Renting a stair lift costs $300 to $500 monthly, making it practical for temporary needs while you wait for funding approvals or determine if a permanent installation makes sense for your situation. Rent-to-own arrangements exist with some suppliers, allowing monthly payments to apply toward eventual ownership if you decide to keep the equipment.
FSA and HSA funds cover stair lift purchases if your doctor provides a prescription establishing medical necessity, offering tax-free dollars that reduce your actual spending. Financing options with promotional zero percent interest plans let you spread costs over 12 to 24 months, making the purchase manageable without depleting savings in a single transaction. Dealer discounts and seasonal promotions happen regularly, so signing up for manufacturer emails alerts you to sales opportunities. Many suppliers offer free consultations and cost estimates, so gathering multiple quotes takes minimal effort and often reveals price differences of $1,000 or more.
Funding Sources Beyond Medicare
The VA’s Home Improvements and Structural Alterations program funds home modifications for eligible veterans regardless of service-related status, covering stair lift costs for those who qualify. Contact your local VA office to discuss eligibility because approval depends on your specific situation and available funding. State Medicaid offices administer Home and Community-Based Services waivers that may cover stair lifts if you meet income and asset limits and if the equipment prevents nursing home placement. Eligibility varies dramatically by state, so contacting your state Medicaid office directly reveals whether this option applies to you.
Area Agencies on Aging connect seniors to local resources, grants, and low-interest loan programs for mobility equipment, and the Eldercare Locator helps you find your nearest agency. Nonprofits like Rebuilding Together and Habitat for Humanity sometimes fund home accessibility modifications for low-income seniors, though availability depends on your location and their current funding. These organizations prioritize aging-in-place projects, making stair lifts eligible for assistance when you qualify based on income. Starting your funding search early matters because approvals take weeks or months, and combining multiple funding sources often fills gaps that no single program covers completely.
Final Thoughts
Getting Medicare stair lift coverage requires three concrete steps: confirming your Medicare Advantage plan covers stair lifts, building medical documentation that demonstrates necessity, and submitting your claim with professional support. Your doctor’s prescription and occupational therapist’s evaluation form the foundation of approval. Without these, your claim fails regardless of how compelling your situation seems. Contact your insurer before spending money on equipment, because pre-authorization requirements vary by plan and purchasing first guarantees out-of-pocket costs.
If you have Original Medicare Part B, stair lifts fall outside coverage because they’re classified as home modifications, not durable medical equipment. Explore alternative funding through the VA if you’re a veteran, your state’s Medicaid HCBS waiver program if you qualify based on income, or Area Agencies on Aging for local resources. These programs move slowly, so starting your application immediately matters. If you have a Medicare Advantage plan, call member services this week and ask directly whether stair lifts qualify for coverage under your specific plan.
Navigating Medicare stair lift coverage alone creates unnecessary delays and mistakes that cost thousands of dollars. The rules differ between Original Medicare and Medicare Advantage plans, between states for Medicaid coverage, and between individual plans within the same insurer. Professional guidance cuts through this complexity and identifies which funding sources actually apply to your situation. Dave Silver Insurance helps people understand their Medicare options and find coverage solutions tailored to their specific needs.
Disclaimer: The information provided in this blog is for general informational purposes only and does not constitute legal, financial, or insurance advice. Coverage options, terms, and availability may vary. Please consult with a licensed professional for advice specific to your situation

